The Vestibular System & Lower Limb Rehab
The most influential system of movement you’re not working with!
RESEARCH ARTICLE
Human movement is no easy feat. We want human movement to be as robust as possible so that it withstands all of the other stressors that we are inevitably going to encounter along the way. This could be as simple as a change in terrain, weaving around people on the street, or picking up speed to a jog to escape an oncoming car as you cross the road. Improving human movement isn’t as simple as a therapist telling you how you should move based on what they think is right and wrong. That is a CONSCIOUS strategy of movement rehabilitation, but we know that the majority of our movement is reflexive and subconscious in nature. As therapists, we don’t exploit these reflexive mechanisms/dynamics enough in people who are suffering with pain and other movement-related problems. What even are these reflexive dynamics? Well, one of the most important reflexive subsystems that has a huge influence on our movement robustness as humans is our Vestibular system. Learning how to easily assess and integrate the Vestibular system during rehab can really help facilitate positive change in pain and other movement-based issues. Keep reading to find out how…
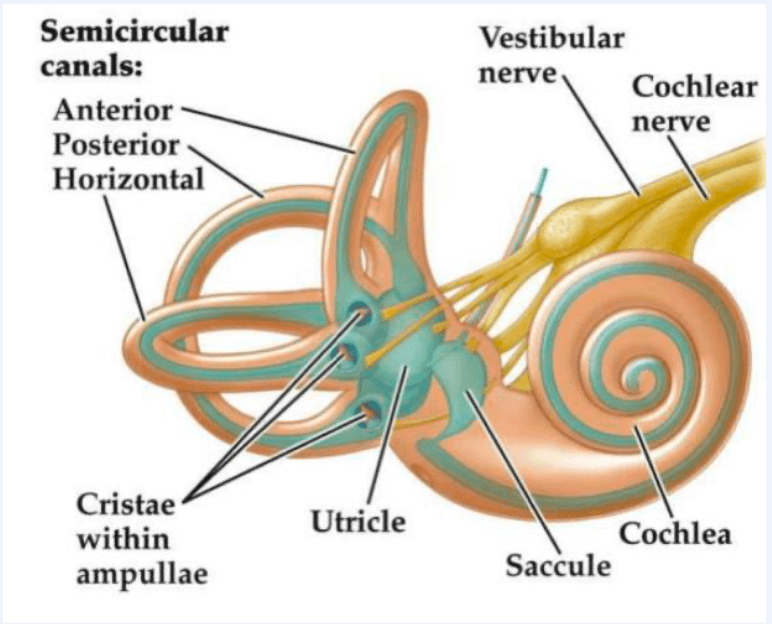
Sifting through neurological research around reflexive mechanisms can be tricky, especially when our goal is to see how it fits in with musculoskeletal rehabilitation. So, our goal is to make that process simple for you, and offer you practical assessment and intervention strategies. In the attached article, researchers set out to understand how reflexive feedback from the leg muscles and inner ear (vestibular system) help to control stance & movement. To put it very simply, our inner ear detects changes in head movement, and with this movement, it creates changes throughout the rest of the body to compensate for the change in head movement. This is crucial to us therapists, because sometimes poor feedback from the vestibular system can lead to EXCESSIVE tone/tension in the muscles around the spine or in the leg muscles, potentially increasing their workload.
In the context of lower limb rehabilitation, first think about what our lower extremities help us to do from a global perspective during human movement. They have a huge role in DECELERATING the movement of our HEAD, ARMS, and TRUNK (HAT). Our HAT makes up two thirds of our body mass. That’s quite a bit of mass to control. During gait, we fall forward and catch ourselves with each step, and so the lower limb muscles need to have the capacity to decelerate the forward motion of the HAT. But, they need help. Remember, we can’t CONSCIOUSLY fire our leg muscles every time we hit the ground, so how do we help the lower limb muscles? Enter the Vestibular system..
As we fall forward during gait, the Vestibular system is the FIRST system to alert our brain that we are falling forward. What do you think is going to happen then? A REFLEXIVE increase in EXTENSOR tone will occur throughout the spinal muscles to help aid in the deceleration, to basically help out the lower limbs. But, if the vestibular system is not doing its job, (and this is a lot more common than you may think) then two responses may occur:
1.) I may default to CONSCIOUSLY bracing my “core”/spinal muscles to aid in movement control (not efficient and a potential reason why your lower back is not going to be very happy if you’re asking it to work overtime/not allowing it to move).
2.) I may have to increase the workload of particular lower limb muscles to decelerate the HAT (not efficient and a potential reason why your piriformis muscle and calves get grumpy).
So, if these REFLEXIVE mechanisms that help decrease the workload of muscles (lower limb muscles in this case) are not helping us out, then we may start to see that constant tension/hypertonicity being expressed in certain areas, and no amount of rubbing, scraping, needling or whatever modality you might use will facilitate long-term change, because the issue is perhaps due to poor top-down communication. Thankfully, integrating the Vestibular system with lower limb rehabilitation is something that we focus on massively during our courses. It doesn’t mean you go straight to the Vestibular system, but once you build load tolerance of the lower limb muscles, you can then integrate it, if your assessment warrants it. The key is looking having a simple assessment process that looks at the three main levels of movement control:
a.) Neural
b.) Muscular
c.) Kinematic
To allow for robust movement, all three of these layers need to HELP EACH OTHER. We need to “share the load.” The first step is identifying if there’s a Vestibular loading discrepancy (if feedback is poor). Now, you’re not going to be able to identify this by looking at someone’s posture, but we need to TEASE out the discrepancy. There are many ways to do this, but a simple place to start is to use your basic gait analysis procedure. This will take you approximately 15 seconds to assess.
Assessment Tip
Ask your client to walk back and forth over a short distance with their EYES OPEN. Then, tell them that you “want to see if the muscles and joints can do their job when we close the eyes. Closing the eyes shifts the workload onto the muscles and joints and other nerves (Don’t say “vestibular system” because they probably don’t know what the hell you mean) and so we may see a difference this time that will help guide our treatment.” By just using the term “nerves,” you are encompassing anything outside of the muscles and joints that contribute to movement control.
Firstly, make sure they are safe to do this. Then, as you watch them walk, do you see them fall slightly or drift to one side? If yes, then this reflects poor communication between the vestibular system and the muscles and joints (particularly around the spine/midline and lower extremity). Of course, a small sway or unsteadiness is normal, but a significant drift to one side indicates a lack of ROBUSTNESS in the Vestibular & muscle/joint communication. Why? Because with the eyes closed, the brain can only rely on the Vestibular system and lower limb/spinal muscles for movement control. If movement control gets significantly worse, then it’s something we definitely need to consider during rehab. It doesn’t mean we jump right into Vestibular loading drills, but it certainly will need to be integrated as part of our graded exposure approach. Keep in mind, this is just a small tweak you can make to identify how other systems aid movement. But, we may need to look a little deeper using other simple assessment tools. If nothing else, using this will help your client come to their own conclusion that there’s more to them than just muscles and joints, but there are other layers that you can both work on together to guide them towards pain-free movement. Help them see that you’re leaving no stone unturned.
